Losing weight conveniently, cheaply, safely. That’s been the holy grail of weight-loss ever since 19th century English undertaker and weight-loss celebrity William Banting’s 1863 Letter on Corpulence spruiked his “miraculous” method of slimming down.
Since then, humans have tried many things – diet, exercise, psychotherapy, surgery – to lose weight. But time and again we return to the promise of a weight-loss drug, whether it’s a pill, injection, or tonic. A “diet drug”.
The history of diet drugs is not a glowing one, however.
There have been so many popular drug treatments for excess weight over the years. All, however, have eventually lost their shine and some have even been banned.
Ozempic is a recent arrival
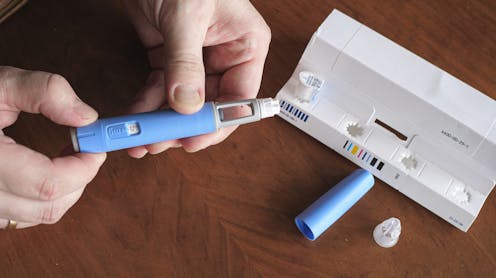
Ozempic and its sister drug Wegovy, both manufactured by Novo Nordisk, are the latest offerings in a long history of drug treatments for people who are overweight. They contain the same active ingredient – semaglutide, which mimics a hormone, GLP-1 (glucagon-like peptide-1) that acts on the hypothalamus (the brain’s “hunger centre”) to regulate appetite.
As an obesity treatment, semaglutide appears to work in part by reducing appetite.
These are injections. And there can be side effects, most commonly nausea and diarrhoea.
Although marketed as treatments for chronic obesity and diabetes, they have exploded in popularity as diet drugs, largely thanks to social media.
This has helped drive a shortage of Ozempic for diabetes treatment.
From ‘gland treatment’ to amphetamines
But Ozempic is not the first weight-loss drug. For example, organotherapy (gland treatment) was hugely popular in the 1920s to 1940s.
It rode on a wave of enthusiasm for endocrinology and specifically the discovery that “ductless glands” – such as the thyroid, pituitary and renal glands – secreted chemical messengers (or “hormones”, as they came to be known).
These hormones coordinate the activities and growth of different parts of the body.
Doctors prescribed overweight people extracts of animal glands – either eaten raw or dried in pill form or injected – to treat their supposedly “sluggish glands”.
For slaughterhouse companies, this was a lucrative new market for offal.
But organotherapy soon fell from favour. There was no evidence excess weight was usually caused by underperforming glands or that gland extracts (thyroid in particular) were doing anything other than poisoning you.
Amphetamines were first used as a nasal decongestant in the 1930s, but quickly found a market for weight-loss.
Why they worked was complex. The drug operated on the hypothalamus but also had an effect on mental state. Amphetamine is, of course, an “upper”.
The theory was it helped people feel up to dieting and gave pleasure not found on a plate. Amphetamines too, fell from treatment use in the 1970s with Nixon’s “war on drugs” and recognition they were addictive.
Another decade, another drug
Each decade seems to produce its own briefly popular weight-loss drug.
For example, the popular diet drug of the 1980s and 90s was fen-phen, which contained appetite suppressants fenfluramine and phentermine.
During the height of its craze, vast numbers of users testified to dramatic weight loss. But after users experienced heart valve and lung disease, fen-phen was withdrawn from the market in 1997. Its producer allocated a reported US$21 billion to settle the associated lawsuits.
The hormone leptin aroused excitement in the mid-1990s. Leptin seemed, for a brief moment, to hold the key to how the hypothalamus regulated fat storage.
Pharmaceutical company Amgen wagered millions buying the rights to the research in the hope this discovery could be turned into a treatment, only to discover it didn’t translate from mice into people. Far from not having enough leptin, people with obesity tend to be leptin-resistant. So taking more leptin doesn’t help with weight-loss. Amgen sold the rights it had paid so much for.
Ephedra was popular as a weight-loss treatment and as a stimulant in the 1990s and 2000s, finding buyers among athletes, body builders and in the military.
But the US Food and Drug Administration banned the sale of dietary supplements containing ephedra in 2004 after it was linked to health problems ranging from heart attacks and seizures to strokes and even death, and in Australia ephedra is prescription-only.
Now we have Ozempic. Just because the history of diet drugs has been so dire, we shouldn’t jump to conclusions about new ones – Ozempic is not a drug of the 1920s or 1960s or 1990s.
And as history recognises, multiple complexities can combine to push a drug into popularity or damn it to history’s rubbish bin.
These include patients’, physicians’ and industry interests; social attitudes about drug treatment; evidence about safety and efficacy; beliefs and knowledge about the cause of excess weight.
One noticeable contrast with past diet drug experiences is that now, many people are happy to talk about using Ozempic. It seems to be increasingly socially acceptable to use a drug to achieve weight-loss for primarily aesthetic reasons.
(Due to Ozempic shortages in Australia, though, doctors have been asked to direct current supplies to people with type 2 diabetes who satisfy certain criteria. In other words, it’s not really meant to be used just to treat obesity).
Our enduring search for weight-loss drugs
Ozempic is predicted to earn Novo Nordisk US$12.5 billion this year alone, but it’s not just industry interests stoking this enduring desire for weight-loss drugs.
Patients on an endless cycle of dieting and exercise want something more convenient, with a more certain outcome. And doctors, too, want to offer patients effective treatment, and a drug prescription is a workable option given the constraints of appointment times.
The body positivity movement has not yet ousted anti-fat bias or stigma. And despite decades of recognition of the major role our physical and social environment plays in human health, there’s little political, public or industry appetite for change.
Individuals are left to personally defend against an obesogenic environment, where economic, cultural, social, health and urban design policies can conspire to make it easy to gain weight but hard to lose it. It is no wonder demand for weight-loss drugs continues to soar.
Read more: Folbigg pardon: science is changing rapidly, and the law needs to change with it
Laura Dawes does not work for, consult, own shares in or receive funding from any company or organization that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.
This article was originally published on The Conversation. Read the original article.








